The shocking statistics behind a new push for better antenatal care for rural, regional and remote women
By Naomi White|
If you're a pregnant woman living in a regional, rural or remote area the statistics are against you.
?Shockingly, the chances of maternal and perinatal death are twice that of major cities. But a new push for better antenatal care is hoping to tackle the issue head on.
One key factor, highlighted in a national survey of GPs and clinicians conducted by researchers at the University of South Australia, in conjunction with The Hospital Research Foundation, was a lack of accessible ultrasounds.?
Now a new program, the Healthy Newborn Project led by chief investigator Associate Professor Nayana Parange and Professor Eva Bezak, and run by University of South Australia lecturer in medical radiation Amber Bidner, is putting the solution in local clinicians' hands.
The initiative trains up local nurses, midwives and GPs to perform point-of-care ultrasounds, allowing the scans to be performed and the results interpreted, on the spot.
READ MORE: 'Raising kids in rural Australia is the hardest, most isolating thing I've ever done in my life'?

Thanks to their efforts, clinicians across some of the most remote and isolated areas in Australia are able to deliver the care those in metro areas take for granted.
One GP, who describes having this knowledge as "life-saving", is Dr Chris ?Clohesy. Based in Mount Isa, the veteran GP spends much of his time travelling to outreach clinics in remote communities across north-west Queensland.
His rounds, so to speak, cover a huge area spanning almost the entirety of the Gulf of Carpentaria. Despite the geographical expanse of the region, and the complex health needs of these communities, he is the only doctor.
"You're by yourself, you're thrown in the deep end and you've got to manage that," says Dr Clohesy. "In remote areas, you don't want to stuff around making a diagnosis. There's only a handful of doctors living in remote communities, it's a difficult gig so to have this training is invaluable."
Before taking part in the training, he was left with two less-than-ideal options should a pregnant woman raise concerns about her pregnancy.
Either he could call for a medical ?retrieval she may not need - a big call given what he says is its near $50,000 price tag, or, if he felt it wasn't urgent, send them home to wait and see. Neither option, unless an obvious emergency, ever sat well with the GP.
It's a story echoed throughout rural, regional and remote areas of Australia. Clinicians in the survey reported a lack of trained staff, staff accessing training and/or access to ultrasound equipment as their biggest obstacles.
READ MORE: Newly pregnant DJ reveals miscarriage heartbreak before baby joy

While for pregnant women, the cost of scans, the travel often involved in seeking these, as well as a lack of transport and childcare were identified as significant barriers.
A lack of understanding about how vital scans are to ensure optimal health outcomes is also of concern. Women in very remote areas were found to be four times more likely than those in outer and inner regional areas to consider ultrasounds unnecessary.
For Bidner, even she admits to being unaware just how dire the lack of antenatal services is.
"I'm from a regional area, and I've worked in rural and remote areas as a nurse. But even as a health professional and doing this research, I wasn't aware myself how bad things are out there," she told 9Honey Parenting.
"Looking at the survey responses and my own pregnancy, and how many appointments and scans are involved, it brought home to me what women go through and the standard of care we take for granted in metropolitan centres."
Bidner said the survey highlighted the reality of the logistical challenges of getting women to appointments, and she was told of women having to travel hours, if not a full day, to access ultrasounds or specialist obstetrics care. ?
READ MORE: Designer brand Balenciaga slammed for promoting 'child fetish content'
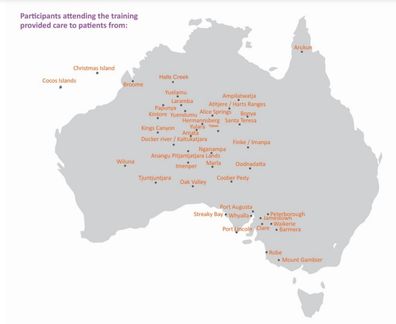
One woman with a high-risk pregnancy had to travel into Adelaide six times alone in the early stages, at six hours travel time per trip.
"Women have to travel long distances or get overnight accommodation or sit on 'bush bus' (a bus servicing remote communities). We've had reports of pregnant women having to get up at dawn to wait for this bus and travel in terrible road conditions to reach antenatal care."
"And there's only one bus a day, so they have to wait the whole day, and in the first trimester when you're not feeling well, or the third when you're very uncomfortable... I can understand why these women aren't going and having antenatal care."
The distance means the women commonly have to do this alone. ?
But timing these scans at crucial points throughout the pregnancy is critical for ensuring better health outcomes. Whether it be to accurately establish due dates �� vital information when you're hours from a hospital, or to time the nuchal translucency scan to pick up any chromosomal abnormalities. And to know when a woman has gone beyond 40 weeks and interventions may be needed.
It's not just a lack of training for clinicians. Often a lack of equipment also means women have to travel further than necessary. Bidner was told of one ultrasound machine being shared by six separate sites.?
READ MORE: 'Our toughest time as parents': Sam and Snez Wood on the traumatic birth of baby Harper?

With nurses and midwives, who are often providing antenatal care in these areas, willing and interested to do the training but put off by the costs of traveling to train and by leaving their clinics unattended, Bidner recently took the training to Alice Springs, following a successful intensive course in Adelaide.
Dr Clohesy, who took part in the Adelaide training tells 9Honey Parenting that knowing how to perform these was life-saving.
"Having this technology right at your fingertips... because I'm the only doctor, if we have a pregnant woman who is bleeding on Mornington Island (a very remote community), you've got to decide, is it a viable pregnancy? Is it a miscarriage? Is the baby doing fine? It's either a $50,000 retrieval to Mount Isa if you're worried it's a miscarriage or it's a 30-second scan on the tummy," he explained.
"If the baby is waving to you it's all good and you're comfortable sitting on that and keeping the woman in the community. That scenario is replayed over and over again. It's so useful to see what's going on. Is the heart rate jumping away, does the placenta look good?"
READ MORE: Mum's heartbreaking warning after baby almost dies from swallowing popular sensory toy?

"Having access as a GP in a remote area to these tools is totally invaluable."
It's not just invaluable from a health perspective. Patients may be hesitant, especially with their first pregnancy, to leave their community. But these scans are a great bonding moment, helping to open up pathways for other antenatal care.
"?When you show mothers the first scan picture, it's a massive rapport connecting moment. They think that you just delivered the baby! It's a really important connector and they may get more confidence in you because of it," Dr Clohesy said.
"And some come in with no idea what their dates are, how far along or when their last period was. You can't tell by looking at their tummy. So I have to work out, do I send them to the big smoke? If it's only five weeks it's too early. But with a scan it's immediately clear."
"It really improved antenatal care of women in pregnancy and the overall mortality rate and for the health of the newborn, because you can see the positioning and how many babies are in there." ?
For a daily dose of 9Honey, subscribe to our newsletter here